What is Cerebral Palsy?
Cerebral Palsy (CP) is “a group of permanent disorders that affect movement and posture”1. The term “Cerebral” refers to the brain and “Palsy” refers to “lack of movement”1. Although CP is a permanent disability, significant functional and life changes can be made with assistance from beneficial therapies.
How many people live with Cerebral Palsy?
The Cerebral Palsy Register Report (2018)2 suggests that:
- 34,000 people in Australia are living with CP
- 1 in 700 Australian children are born with CP
- 1 in 2 people living with CP experiences chronic pain
- 1 in 3 people living with CP can’t walk
- 1 in 4 people living with CP can’t speak
- By 2050, it is expected that 47,601 people in Australia will be living with CP
Does Cerebral Palsy just affect movement?
There are many different types and presentations of CP. Even though CP is generally characterised by affected movement, the way people living with CP think, feel, behave and communicate can also be affected3.
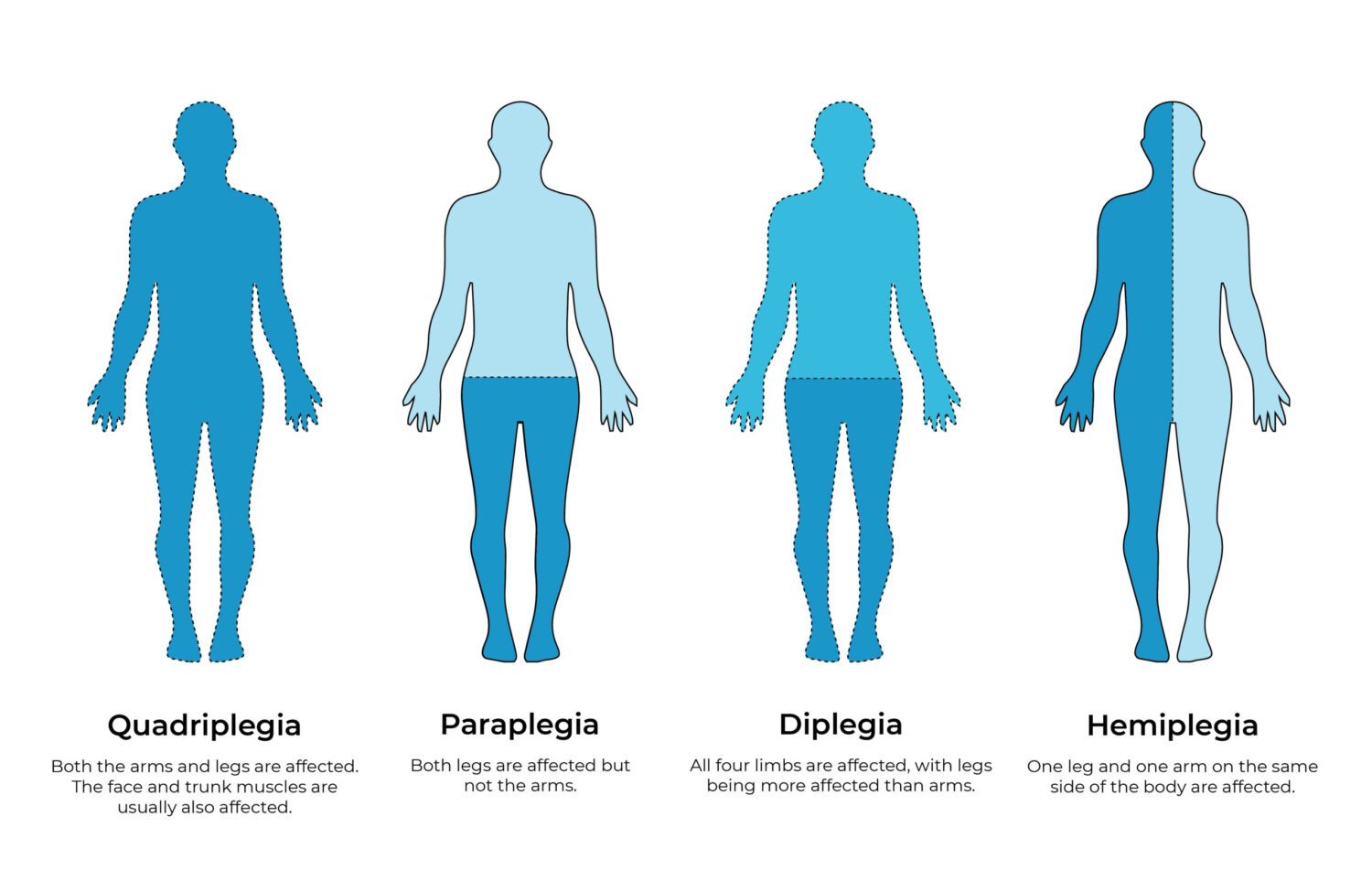
What part of the body does Cerebral Palsy affect?
CP affects different people in different ways. Some people may develop a minor presentation, whereas others may be more physically impaired.
We can classify CP into four different categories based on areas of the body affected:
What are the different types of Cerebral Palsy?
The affected limbs can present in different ways. There are four main types of CP:
- Spastic CP – Stiffness or tightness of the muscle group. Muscular stiffness then makes the muscle weak and people living with Spastic CP often have problem with walking and posture. Spasticity is the most common type of CP with 85-91% of people experiencing this type.
- Dyskinetic (Athetoid) CP – Characterised by uncontrolled movements. Movements usually alternate from slow to rapid. Dyskinetic CP is not as common as spasticity with 4-7% of people experiencing this type.
- Ataxic CP – Characterised by shaky movements with reduced balance and stability. People living with Ataxic CP will often have difficulty coordinating movements and lack depth perception. 4-6% of people experience Ataxic CP.
- Mixed CP – When the person experiences more than one type of CP. Mixed CP is very rare.
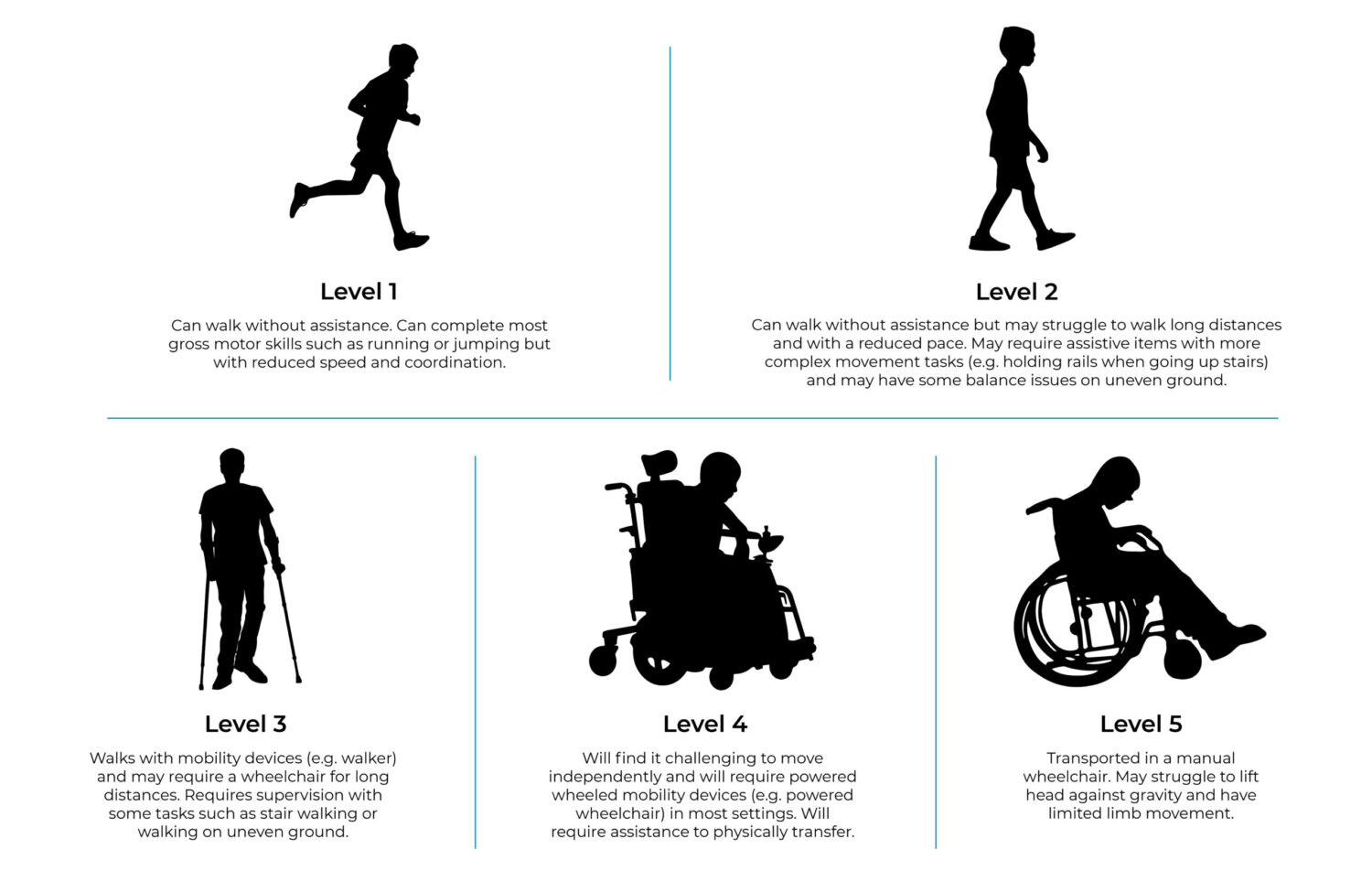
How do we classify the movement functions of Cerebral Palsy?
There are five levels that we use to classify a person living with CP’s ability to move, otherwise known as the Gross Motor Function Classification System (GMFCS). Understanding these classifications helps us to prescribe more individualised treatment plans.
Classifications of gross motor functions:
Why is exercise important for Cerebral Palsy?
People living with CP have reduced physical activity levels compared to peers without disability4. Reduced access to the benefits of exercise can have serious health implications in the future. Although CP does not get necessarily worse with age, between 20-50% of people living with CP experience a deterioration in mobility as they enter adulthood5. When a person finds it more challenging to move and access the benefits of exercise, they are more likely to have reduced cardiovascular health, general strength, less range of motion, an increase in existing pain levels and potentially balance issues6.
The reduced ability to engage in exercise results in low muscle mass and low muscle strength that predisposes the person to sarcopenia7. Adults living with CP are twice as likely to develop heart failure, high blood pressure and asthma asthma and five times more likely to have a stroke8.
Exercise is medicine has never been more true for people living with CP. By engaging in regular physical activity/exercise, we are able to build up strength and fitness that can significantly reduce the chances of adverse health outcomes occurring.
Exercise not only plays a role in improving overall health, but is vital for improving physical function and independence. Building up the person’s ability to engage in meaningful activities and using exercise to help with activities of daily life will help improve the person’s quality of life. Exercise also provides an opportunity to build confidence through movement and can help to change the person’s perception of their physical ability.
An exercise professional has the skills and knowledge to design individualised exercise programs for people living with all types of CP to ensure that they have access to the benefits of exercise.